An optic nerve which is damaged, most often following too high pressure inside the eye. And a field of vision that narrows, from the periphery to the center. This is the definition of glaucoma, for which 1.5 million French people are currently monitored or treated.
Medications, lasers or surgery allow the majority of them to stabilize the disease at the stage where it was discovered. But for 10 to 15 percent of sufferers, glaucoma continues to worsen and can lead to blindness. Hence all-out research to protect the optic nerve.
“No treatment directly aimed at the regeneration of these nerve fibers has yet proven its effectiveness in humans,” warns Professor Christophe Baudouin, of the Quinze-Vingts-Institut de la vision hospital, “but there are has made many advances in the control of intraocular pressure. This neuroprotection strategy has largely demonstrated its effectiveness.
Silent for years, glaucoma is, in most cases, linked to problems with defective evacuation of aqueous humor. Continuously secreted by glands located near the lens, it accumulates inside the eye, increases pressure and destroys the nerve cells of the optic nerve. To remedy this, once the diagnosis has been made, “we have four therapeutic families, a fifth currently the subject of clinical trials,” continues the professor.
Some medications reduce the secretion of aqueous humor, others facilitate its flow outside the eye through a drainage system called the “trabecular meshwork”. With one exception, they are administered as eye drops. However, except for surgery, these are prescribed for life. In view of their potential deleterious effects on the ocular surface - dryness, irritation, inflammation - the recent development of preservative-free formulas has constituted a formidable advance. And when they prove insufficient, we resort to laser or surgical interventions, the technique of which has also progressed.
“The laser makes it possible to remove the blockage by creating a small orifice in the iris, for so-called “closed angle” glaucoma,” explains Professor Baudouin. It can also improve the functioning of the trabecular meshwork for open-angle glaucoma, which is the most common. These objectives are also those of surgery, in patients whose disease is not stabilized by eye drops or lasers. “Over the past ten years, it has become less risky, thanks to so-called minimally invasive procedures based on the implantation of microdrains to evacuate aqueous humor,” adds the ophthalmologist. However, there remain patients for whom all these therapies are not enough. Hence the exploration of other avenues targeting the optic nerve more directly.
“A few years ago, I would have told you that I hoped to obtain good results with stem cell injections,” recognizes Christophe Baudouin. “But preclinical trials have shown the high variability of responses to this treatment, and especially its dangerousness for the eye.” Another option considered: the use of gene therapy, to produce a neuroprotective protein in the eye.
Finally, we are also considering intervening in the visual cortex, by stimulating genetically modified neurons to be activated by ultrasound, hence the name “sonogenetic therapy”. Currently, these treatments are only tested in animals. But scientists are hopeful of achieving human trials in the near future.

 Gaza: under the spotlight, the Israeli-Palestinian conflict shakes up the Eurovision contest
Gaza: under the spotlight, the Israeli-Palestinian conflict shakes up the Eurovision contest Black soldier killed by a police officer in the United States: the sheriff publishes the video of the arrest
Black soldier killed by a police officer in the United States: the sheriff publishes the video of the arrest In Malmö, the Eurovision party transformed into entrenched camps
In Malmö, the Eurovision party transformed into entrenched camps In Russia, Vladimir Putin stigmatizes “Western elites”
In Russia, Vladimir Putin stigmatizes “Western elites” “Mediterranean diet” or “DASH”, two good tips for eating better
“Mediterranean diet” or “DASH”, two good tips for eating better Fatal case of cholera in Mayotte: the epidemic is “contained”, assures the government
Fatal case of cholera in Mayotte: the epidemic is “contained”, assures the government The presence of blood in the urine, a warning sign of bladder cancer
The presence of blood in the urine, a warning sign of bladder cancer A baby whose mother smoked during pregnancy will age more quickly
A baby whose mother smoked during pregnancy will age more quickly Artificial intelligence lies, cheats and deceives us, and that's a problem, experts warn
Artificial intelligence lies, cheats and deceives us, and that's a problem, experts warn Google Cloud mistakenly deletes UniSuper fund account and deprives 600,000 Australians of their superannuation
Google Cloud mistakenly deletes UniSuper fund account and deprives 600,000 Australians of their superannuation IBM, Amazon, Hager... These record investments expected at the Choose France summit
IBM, Amazon, Hager... These record investments expected at the Choose France summit Boeing's black streak: a second Air France flight diverted in three days for “a smell of heat”
Boeing's black streak: a second Air France flight diverted in three days for “a smell of heat” Paola Locatelli: “Influence is comfortable but cinema gives me adrenaline”
Paola Locatelli: “Influence is comfortable but cinema gives me adrenaline” Swifties attack hotels in Lyon
Swifties attack hotels in Lyon Radical Optimism by Dua Lipa, a tangy album in half-tone
Radical Optimism by Dua Lipa, a tangy album in half-tone Peter Weir rewarded for his career with an honorary Golden Lion at the Venice Film Festival in September
Peter Weir rewarded for his career with an honorary Golden Lion at the Venice Film Festival in September Omoda 7, another Chinese car that could be manufactured in Spain
Omoda 7, another Chinese car that could be manufactured in Spain BYD chooses CA Auto Bank as financial partner in Spain
BYD chooses CA Auto Bank as financial partner in Spain Tesla and Baidu sign key agreement to boost development of autonomous driving
Tesla and Baidu sign key agreement to boost development of autonomous driving Skoda Kodiaq 2024: a 'beast' plug-in hybrid SUV
Skoda Kodiaq 2024: a 'beast' plug-in hybrid SUV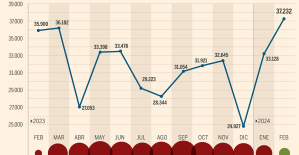 The home mortgage firm rises 3.8% in February and the average interest moderates to 3.33%
The home mortgage firm rises 3.8% in February and the average interest moderates to 3.33%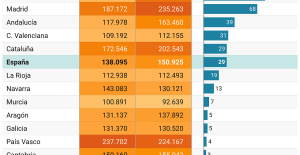 This is how housing prices have changed in Spain in the last decade
This is how housing prices have changed in Spain in the last decade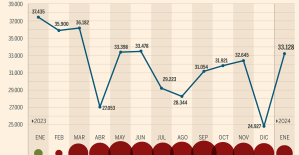 The home mortgage firm drops 10% in January and interest soars to 3.46%
The home mortgage firm drops 10% in January and interest soars to 3.46% The jewel of the Rocío de Nagüeles urbanization: a dream villa in Marbella
The jewel of the Rocío de Nagüeles urbanization: a dream villa in Marbella Diving into the secrets of the National Assembly
Diving into the secrets of the National Assembly Institutions: senators want to restore the accumulation of mandates and put an end to the automatic presence of ex-presidents on the Constitutional Council
Institutions: senators want to restore the accumulation of mandates and put an end to the automatic presence of ex-presidents on the Constitutional Council Europeans: David Lisnard expresses his “essential and vital” support for François-Xavier Bellamy
Europeans: David Lisnard expresses his “essential and vital” support for François-Xavier Bellamy Facing Jordan Bardella, the popularity match turns to Gabriel Attal’s advantage
Facing Jordan Bardella, the popularity match turns to Gabriel Attal’s advantage These French cities that will boycott the World Cup in Qatar
These French cities that will boycott the World Cup in Qatar Bundesliga: 50th match without defeat for Leverkusen, big winner in Bochum
Bundesliga: 50th match without defeat for Leverkusen, big winner in Bochum Football: Choupo-Moting and Sarr leave Bayern Munich
Football: Choupo-Moting and Sarr leave Bayern Munich Top 14: Toulouse wins the duel of the leaders against Stade Français and takes the lead in the ranking
Top 14: Toulouse wins the duel of the leaders against Stade Français and takes the lead in the ranking Ligue 1: PSG surprised for Mbappé's last at the Parc, Monaco officially in the Champions League
Ligue 1: PSG surprised for Mbappé's last at the Parc, Monaco officially in the Champions League


















