These decisions were a sign of an increase in the pandemic in many Western countries that are struggling to convince people to get vaccinated.
After St. Luke's Health System in Idaho, the largest hospital network in Idaho, requested that state health officials allow "crisis standard of care" due to the state's inability to provide medical treatment for the increased COVID-19 patient population.
Idaho has only 40% of its residents who are fully vaccinated against COVID-19, making it one of the least-vaccinated states in America.
According to crisis care standards, ICU beds and other scarce resources will only be given to patients who are most likely to survive. Others will be treated using less effective methods, or in extreme cases, pain relief and palliative care.
In response to a rise in COVID-19-related patients, a Helena hospital had to adopt crisis care standards. Officials said that St. Peter's Health hospital has reached its maximum capacity for critical care.
Providence Alaska Medical Center in Alaska, the largest hospital in Alaska, started prioritizing its resources earlier this week.
Thursday's action in Idaho was made one week after officials in Idaho allowed health care rationing in hospitals located in the northern part of the state.
"The situation is dire - we don't have sufficient resources to adequately treat patients in our hospitals.
He encouraged people to be vaccinated, and to wear masks indoors as well as in crowded outdoor environments.
Jeppesen stated, "Our hospitals need our help."
According to Dr. Jim Souza, chief medical officer, patients in Idaho's St. Luke's Health System are ventilated manually by a nurse or doctor using a bag to hold them. This can last up to an hour while hospital officials search for a bed with a ventilator.
Some patients are being treated in high-flow oxygen rooms that do not have monitoring systems. This means that a nurse or doctor might not be able to hear the alarm if there is a medical emergency. Patients are being treated in waiting rooms at emergency departments for life-threatening infections such as sepsis.
Souza stated that the normal standards of care are a safety net that allows doctors to perform "high wire acts" such as open heart surgery, bone marrow transplants, and neuro-interventional stroke treatment. "The net is gone and people will fall off the high wire," Souza said.
According to Johns Hopkins University, one in 201 Idahoans tested positive for COVID-19 during the week. For newly confirmed cases per capita, the mostly rural state is 12th in the United States.
Hospitalizations have risen dramatically. According to the latest state data, 678 people were admitted to hospital for coronavirus on Monday.
The number of COVID-19-infant patients in ICU beds at 170 each day has remained steady for the past two weeks, suggesting that the state may be reaching its limit in treating ICU patients.
All state hospitals are now allowed to ration medical care as necessary, but some may not be able to do so. Public health officials stated that each hospital will determine how to implement crisis standards of care within its facility.
Nearly 92% of COVID-19 patients in St. Luke’s hospitals were not vaccinated on Wednesday. Sixty-one out of the hospital's total 78 ICU patients were unvaccinated. St. Luke's doctors have been pleading with Idahoans for months to get vaccinated. They also warned that hospitals were rapidly running out beds.
The crisis in health care is not just affecting hospitals; primary care physicians as well as medical equipment suppliers are also experiencing difficulties with coronavirus-related demand.
Norco Medical, a major supplier of medical equipment, stated that the demand for oxygen tanks has increased and sometimes forced them to send patients home without as many cylinders as they normally would. Elias Margonis, President of Norco Medical, stated that high-flow oxygen equipment is being requested more often for patients at home. This equipment is normally used in hospitals or hospice care.
Margonis stated that it seemed like they were releasing patients aggressively in order to make room for new patients.
Margonis spent much time calling hospital leaders and public health officials to discuss how the new crisis standards of care would affect the discharge process for patients from hospitals. He said that the company already has seen an increase of customers who are interested in specialty oxygen equipment that can flow at 8-12 or 20 liters per hour, rather than the usual 4 or 5 liters.
Margonis stated, "When someone goes home we bring their bed and wheelchair, we take their cannula, our oxygen, and we bring their bed." "This is what we are trying to say. You can't just let the problem go, even if they're on the mend or on their way to recovery. They need support to recover.
Primary Health Medical Group in Idaho, Idaho's largest independent primary and urgent care, was forced to reduce its operating hours due to the high demand for patients. Staffers had to stay open until closing to ensure that all of them were seen. The company was also dealing with sicker staffers who had been exposed to coronavirus or were suffering from symptoms, and were waiting for tests.
The medical group is now preparing to monitor patients being released earlier than usual or trying to avoid emergency room completely. CEO Dr. David Peterman said that they will likely be more sick and require more care.
"This is heartbreaking. He said that he has been practicing medicine in southwest Idaho for over 40 years and had never seen anything similar.

 United States: divided on the question of presidential immunity, the Supreme Court offers respite to Trump
United States: divided on the question of presidential immunity, the Supreme Court offers respite to Trump Maurizio Molinari: “the Scurati affair, a European injury”
Maurizio Molinari: “the Scurati affair, a European injury” Hamas-Israel war: US begins construction of pier in Gaza
Hamas-Israel war: US begins construction of pier in Gaza Israel prepares to attack Rafah
Israel prepares to attack Rafah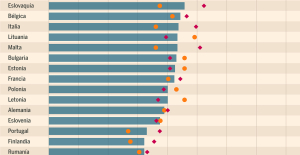 Spain is the country in the European Union with the most overqualified workers for their jobs
Spain is the country in the European Union with the most overqualified workers for their jobs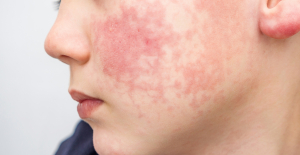 Parvovirus alert, the “fifth disease” of children which has already caused the death of five babies in 2024
Parvovirus alert, the “fifth disease” of children which has already caused the death of five babies in 2024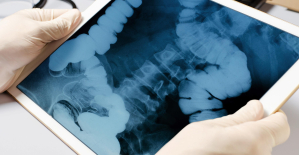 Colorectal cancer: what to watch out for in those under 50
Colorectal cancer: what to watch out for in those under 50 H5N1 virus: traces detected in pasteurized milk in the United States
H5N1 virus: traces detected in pasteurized milk in the United States Private clinics announce a strike with “total suspension” of their activities, including emergencies, from June 3 to 5
Private clinics announce a strike with “total suspension” of their activities, including emergencies, from June 3 to 5 The Lagardère group wants to accentuate “synergies” with Vivendi, its new owner
The Lagardère group wants to accentuate “synergies” with Vivendi, its new owner The iconic tennis video game “Top Spin” returns after 13 years of absence
The iconic tennis video game “Top Spin” returns after 13 years of absence Three Stellantis automobile factories shut down due to supplier strike
Three Stellantis automobile factories shut down due to supplier strike A pre-Roman necropolis discovered in Italy during archaeological excavations
A pre-Roman necropolis discovered in Italy during archaeological excavations Searches in Guadeloupe for an investigation into the memorial dedicated to the history of slavery
Searches in Guadeloupe for an investigation into the memorial dedicated to the history of slavery Aya Nakamura in Olympic form a few hours before the Flames ceremony
Aya Nakamura in Olympic form a few hours before the Flames ceremony Psychiatrist Raphaël Gaillard elected to the French Academy
Psychiatrist Raphaël Gaillard elected to the French Academy Skoda Kodiaq 2024: a 'beast' plug-in hybrid SUV
Skoda Kodiaq 2024: a 'beast' plug-in hybrid SUV Tesla launches a new Model Y with 600 km of autonomy at a "more accessible price"
Tesla launches a new Model Y with 600 km of autonomy at a "more accessible price" The 10 best-selling cars in March 2024 in Spain: sales fall due to Easter
The 10 best-selling cars in March 2024 in Spain: sales fall due to Easter A private jet company buys more than 100 flying cars
A private jet company buys more than 100 flying cars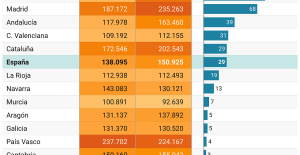 This is how housing prices have changed in Spain in the last decade
This is how housing prices have changed in Spain in the last decade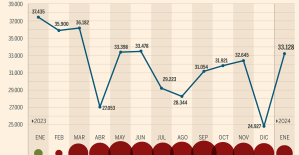 The home mortgage firm drops 10% in January and interest soars to 3.46%
The home mortgage firm drops 10% in January and interest soars to 3.46% The jewel of the Rocío de Nagüeles urbanization: a dream villa in Marbella
The jewel of the Rocío de Nagüeles urbanization: a dream villa in Marbella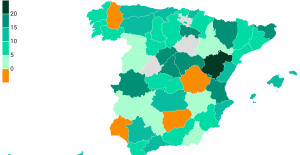 Rental prices grow by 7.3% in February: where does it go up and where does it go down?
Rental prices grow by 7.3% in February: where does it go up and where does it go down? Even on a mission for NATO, the Charles-de-Gaulle remains under French control, Lecornu responds to Mélenchon
Even on a mission for NATO, the Charles-de-Gaulle remains under French control, Lecornu responds to Mélenchon “Deadly Europe”, “economic decline”, immigration… What to remember from Emmanuel Macron’s speech at the Sorbonne
“Deadly Europe”, “economic decline”, immigration… What to remember from Emmanuel Macron’s speech at the Sorbonne Sale of Biogaran: The Republicans write to Emmanuel Macron
Sale of Biogaran: The Republicans write to Emmanuel Macron Europeans: “All those who claim that we don’t need Europe are liars”, criticizes Bayrou
Europeans: “All those who claim that we don’t need Europe are liars”, criticizes Bayrou These French cities that will boycott the World Cup in Qatar
These French cities that will boycott the World Cup in Qatar Archery: everything you need to know about the sport
Archery: everything you need to know about the sport Handball: “We collapsed”, regrets Nikola Karabatic after PSG-Barcelona
Handball: “We collapsed”, regrets Nikola Karabatic after PSG-Barcelona Tennis: smash, drop shot, slide... Nadal's best points for his return to Madrid (video)
Tennis: smash, drop shot, slide... Nadal's best points for his return to Madrid (video) Pro D2: Biarritz wins a significant success in Agen and takes another step towards maintaining
Pro D2: Biarritz wins a significant success in Agen and takes another step towards maintaining


















