For the third time in the world, a cancer patient with HIV has been successfully cured of both diseases with the help of a stem cell transplant. This is reported by physicians from the University Hospital Düsseldorf in the journal "Nature Medicine". After such a therapy had already been used successfully in the "Berlin patient" and the "London patient", the research team hopes to find treatment options for HIV-infected people without cancer and is relying on gene therapy approaches. However, independent experts still see serious obstacles.
In 2011, three years after his HIV diagnosis, the “Düsseldorf patient” was diagnosed with acute myeloid leukemia (AML) – a form of blood cancer. In 2013 he received a stem cell transplant. "Right from the start, the aim of the transplantation was to get both the leukemia and the HI virus under control," explained Guido Kobbe from the University Hospital Düsseldorf, who carried out the operation.
The stem cells - like those of two comparable cases from Berlin and London - had a specific gene mutation called CCR5Δ32 (CCR5-Delta32). This mutation, which occurs mainly in people from Northern and Central Europe but is very rare overall, means that there is no docking point for HIV on the immune cells. Without such a docking point, the virus cannot find an entry point and cannot infect the cells, which makes carriers of the mutation almost resistant to the pathogen.
In fact, the transplant resulted in remission of HIV symptoms, so in 2018 the treatment team decided to discontinue antiviral HIV therapy. The subsequent monitoring of the patient over several years proved the continuing success: Today the scientists speak of a complete recovery of the meanwhile 53-year-old.
Björn Jensen, part of the international team of doctors, summed up: "After our intensive research, we can now confirm that it is fundamentally possible to prevent the multiplication of the HI virus in the long term by combining two essential methods." On the one hand, this is the extensive emptying of the Virus reservoirs in long-lived immune cells and, on the other hand, the transfer of HIV resistance from the donor immune system to the recipient. "So the HI virus has no chance of multiplying again."
However, such a therapy is currently only possible for a few patients: on the one hand, because the number of suitable donors with the mutation is so small. On the other hand, because stem cell transplantation can only be used in the context of the treatment of other life-threatening diseases such as cancer due to the many risks.
The research team therefore hopes that the study will show ways of treating HIV in the future by transplanting gene-edited stem cells to infected people without cancer. The mutation would be inserted, for example, using gene scissors such as Crispr/Cas and combined with strategies that reduce the HIV reservoirs in the body.
According to Jürgen Rockstroh from the University Hospital Bonn, there is still a long way to go. An expansion of the therapeutic approach to HIV-infected people without cancer remains unrealistic for the time being. "One problem here seems to be that with appropriate gene therapy approaches, all cells must subsequently show the CCR5 gene mutation," explained Rockstroh.
However, this is not necessarily achievable for all cells, so that there always remains a reservoir of cells that have not been modified by gene therapy. "Nevertheless, there are also individual cases after gene therapy that show at least better control of the HI viremia after stopping the HIV therapy, so that it is certainly promising to continue researching gene therapy approaches."
According to Boris Fehse from the Hamburg-Eppendorf University Hospital, these approaches include protecting blood cells from HIV or even cutting the virus out of infected cells. With regard to the hope described by the authors, the biomedical scientist also refers to the small number of suitable stem cell donors, possible rejection reactions and side effects, but is nevertheless optimistic.
"It is very easy to imagine that in the near future HIV patients who need a stem cell transplant because of blood cancer will always be offered the opportunity to have the transplant treated with gene scissors before the infusion," says Fehse. Depending on the disease, these could be donor or the patient's own blood stem cells.
As Toni Cathomen from the University Hospital Freiburg added, HIV-infected people with well-adjusted therapy now have a life expectancy that is similar to that of the general population anyway: In his opinion, the risk that is currently associated with a stem cell transplant is therefore currently for "healthy" HIV-infected people not justifiable.
But that could change in the future, according to the molecular biologist. Because: "In contrast to conventional HIV therapy, which has to be taken for life, the genetic approach promises a cure after a single use of gene scissors, i.e. a complete remission, and thus the discontinuation of antiretroviral therapy."
"Aha! Ten minutes of everyday knowledge" is WELT's knowledge podcast. Every Tuesday and Thursday we answer everyday questions from the field of science. Subscribe to the podcast on Spotify, Apple Podcasts, Deezer, Amazon Music, among others, or directly via RSS feed.

 War in Ukraine: when kyiv attacks Russia with inflatable balloons loaded with explosives
War in Ukraine: when kyiv attacks Russia with inflatable balloons loaded with explosives United States: divided on the question of presidential immunity, the Supreme Court offers respite to Trump
United States: divided on the question of presidential immunity, the Supreme Court offers respite to Trump Maurizio Molinari: “the Scurati affair, a European injury”
Maurizio Molinari: “the Scurati affair, a European injury” Hamas-Israel war: US begins construction of pier in Gaza
Hamas-Israel war: US begins construction of pier in Gaza First three cases of “native” cholera confirmed in Mayotte
First three cases of “native” cholera confirmed in Mayotte Meningitis: compulsory vaccination for babies will be extended in 2025
Meningitis: compulsory vaccination for babies will be extended in 2025 Spain is the country in the European Union with the most overqualified workers for their jobs
Spain is the country in the European Union with the most overqualified workers for their jobs Parvovirus alert, the “fifth disease” of children which has already caused the death of five babies in 2024
Parvovirus alert, the “fifth disease” of children which has already caused the death of five babies in 2024 Inflation rebounds in March in the United States, a few days before the Fed meeting
Inflation rebounds in March in the United States, a few days before the Fed meeting Video games: Blizzard cancels Blizzcon 2024, its annual high mass
Video games: Blizzard cancels Blizzcon 2024, its annual high mass Falling wings of the Moulin Rouge: who will pay for the repairs?
Falling wings of the Moulin Rouge: who will pay for the repairs? “You don’t sell a company like that”: Roland Lescure “annoyed” by the prospect of a sale of Biogaran
“You don’t sell a company like that”: Roland Lescure “annoyed” by the prospect of a sale of Biogaran Exhibition: in Deauville, Zao Wou-Ki, beauty in all things
Exhibition: in Deauville, Zao Wou-Ki, beauty in all things Dak’art, the most important biennial of African art, postponed due to lack of funding
Dak’art, the most important biennial of African art, postponed due to lack of funding In Deadpool and Wolverine, Ryan and Hugh Jackman explore the depths of the Marvel multiverse
In Deadpool and Wolverine, Ryan and Hugh Jackman explore the depths of the Marvel multiverse Tom Cruise returns to Paris for the filming of Mission Impossible 8
Tom Cruise returns to Paris for the filming of Mission Impossible 8 Skoda Kodiaq 2024: a 'beast' plug-in hybrid SUV
Skoda Kodiaq 2024: a 'beast' plug-in hybrid SUV Tesla launches a new Model Y with 600 km of autonomy at a "more accessible price"
Tesla launches a new Model Y with 600 km of autonomy at a "more accessible price" The 10 best-selling cars in March 2024 in Spain: sales fall due to Easter
The 10 best-selling cars in March 2024 in Spain: sales fall due to Easter A private jet company buys more than 100 flying cars
A private jet company buys more than 100 flying cars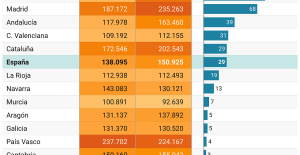 This is how housing prices have changed in Spain in the last decade
This is how housing prices have changed in Spain in the last decade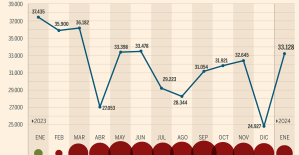 The home mortgage firm drops 10% in January and interest soars to 3.46%
The home mortgage firm drops 10% in January and interest soars to 3.46% The jewel of the Rocío de Nagüeles urbanization: a dream villa in Marbella
The jewel of the Rocío de Nagüeles urbanization: a dream villa in Marbella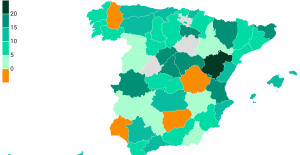 Rental prices grow by 7.3% in February: where does it go up and where does it go down?
Rental prices grow by 7.3% in February: where does it go up and where does it go down? Even on a mission for NATO, the Charles-de-Gaulle remains under French control, Lecornu responds to Mélenchon
Even on a mission for NATO, the Charles-de-Gaulle remains under French control, Lecornu responds to Mélenchon “Deadly Europe”, “economic decline”, immigration… What to remember from Emmanuel Macron’s speech at the Sorbonne
“Deadly Europe”, “economic decline”, immigration… What to remember from Emmanuel Macron’s speech at the Sorbonne Sale of Biogaran: The Republicans write to Emmanuel Macron
Sale of Biogaran: The Republicans write to Emmanuel Macron Europeans: “All those who claim that we don’t need Europe are liars”, criticizes Bayrou
Europeans: “All those who claim that we don’t need Europe are liars”, criticizes Bayrou These French cities that will boycott the World Cup in Qatar
These French cities that will boycott the World Cup in Qatar Basketball: Strasbourg appeals the victory recovered by Monaco
Basketball: Strasbourg appeals the victory recovered by Monaco Top 14: UBB with Tatafu and Moefana against Bayonne
Top 14: UBB with Tatafu and Moefana against Bayonne MotoGP: Bagnaia dominates qualifying practice in Spain and sets track record
MotoGP: Bagnaia dominates qualifying practice in Spain and sets track record Olympic Games: in Athens, Greece transmits the Olympic flame to France
Olympic Games: in Athens, Greece transmits the Olympic flame to France