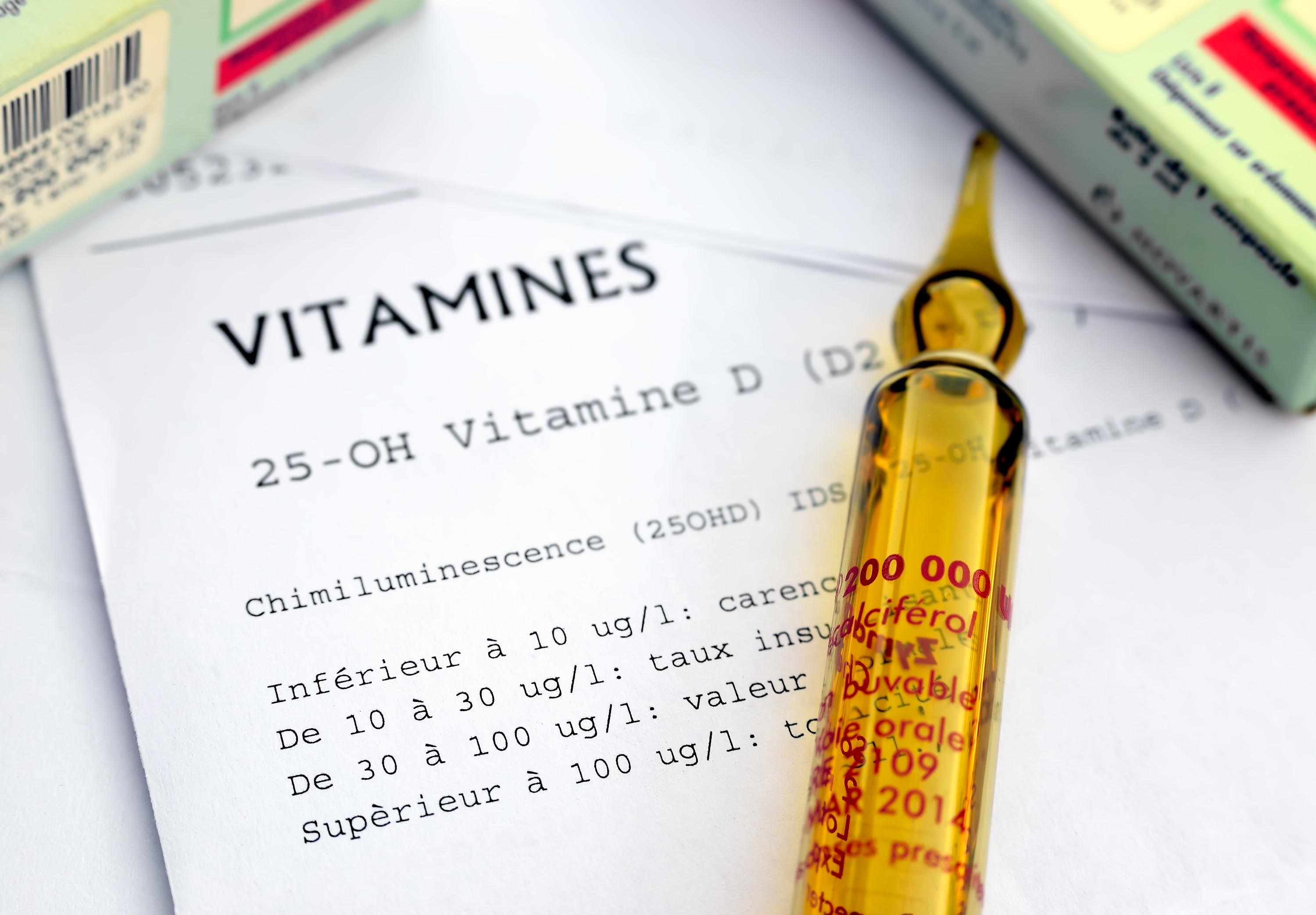
It is one of the best-selling drugs in France, according to Social Security databases, and links have been established between vitamin D deficiency and many diseases. Some people would like to prescribe it to everyone, especially during winter. But are we really all deficient in vitamin D? Does this supposed deficit give rise to many diseases? Should you supplement? “Le Figaro” takes stock.
Vitamin D plays an essential role in the absorption of calcium by the intestine, and by the kidneys of calcium and phosphorus. It is therefore essential for good bone mineralization, and its lack can be responsible for rickets in children (with growth delays and bone deformities), and osteomalacia (“soft” bone) or (but this point is controversial) osteoporosis (less dense bone) in adults. More recently, research has identified vitamin D receptors in most tissues of the body; it would therefore be involved in numerous physiological processes and would have anti-infectious, anti-inflammatory, anti-tumor and cardiovascular effects.
It is found in certain foods, but "the body's vitamin D comes 80-90% from skin biosynthesis under the effect of ultraviolet (UV) radiation from the sun", recalled the High Council for Public Health (HCSP ) in an opinion published in 2022. It is synthesized in our skin, from a cholesterol derivative; under the effect of UV rays, it transforms into a molecule called cholecalciferol. This is metabolized by the liver into 25-hydroxy-vitamin D (the molecule sought in blood tests of vitamin D), then by the kidney into 1-25-dihydroxy-vitamin D (the active form of vitamin D). Combined with a balanced diet, simple exposure of the forearms and face for a few minutes to a few tens of minutes two to three times a week, depending on the amount of sunlight and the color of the skin, would be enough to meet the needs of most people. 'between us.
In the general population, we are talking about a deficiency below 10 nanograms per milliliter of blood of 25-hydroxy-vitamin D (1 nanogram is a billionth of a gram), and an insufficiency between 10 and 20 ng/ml. The HCSP specifies that, “for the sake of caution, the maximum concentration (…) not to be exceeded is currently set between 50 and 60 ng/ml”. In the general population, 4% to 6% of French adults are deficient, and 40% to 50% are deficient. And 80% are below 30 ng/ml, and considered in deficit by some experts. Can such a large part of the population really be deficient in such an essential vitamin without worrying the public authorities?
In reality, these thresholds come from opinions of groups of experts on relatively fragile bases, and they are contested, in particular that of 30 ng/ml. Especially since one of the popes of vitamin D in the United States, editor of American guidelines on the subject, was singled out for his links with vitamin D manufacturers. In 2011, a few months after a report from the American Academy of Medicine who estimated that the vast majority of Americans did not need vitamin D supplementation or dosing, Boston University endocrinologist Michel Holick oversaw a report on behalf of the Endocrine Society to the findings radically different, which serves as recommendations in the United States. However, Dr. Holick, reported in 2018 by the New York Times, admitted to having been largely paid as an expert by the pharmaceutical industry and producers of food supplements, and to having received research funds from manufacturers of UV cabins. He defended himself by asserting that this had not influenced his scientific considerations on the subject, but it casts at least an insistent shadow on the sincerity of his positions.
Another subject of distrust: the reliability and usefulness of vitamin D dosages, which are not easy to carry out and are poorly standardized, which complicates the comparison of two results obtained in two different laboratories.
In France, the High Authority for Health (HAS) reserves them for 6 specific clinical situations (suspected rickets or osteomalacia, monitoring of adults with kidney transplants, before and after bariatric surgery, elderly people prone to repeated falls, taking of medications recommending the measurement of vitamin D). Outside of these situations, their cost must be borne by the patient according to Health Insurance, for whom they are very expensive: 6.8 million dosages representing a cost of 41.7 million euros were carried out in the private laboratories in 2022, compared to 3.9 million in 2015, it highlighted last July in its “Expenses and income report for 2024”. 90% of dosages carried out in 16-65 year olds would have been wrongly prescribed and did not comply with HAS recommendations.
Cancers, cardiovascular diseases, fractures, stroke, kidney diseases, multiple sclerosis, Alzheimer's disease or more recently Covid-19... Many studies have established links between vitamin D deficiency and poor health. But they only establish a statistical link between the two, without allowing us to know whether we fall ill because we lack vitamin D, or whether we lack it because of a poor state of health. Many teams have sought to supplement patients in the hope that this would improve their health, but almost all large, well-conducted trials have failed to show an effect, including in populations with a deficiency at the start of the study. Some seemed to favor a positive effect, which was later denied. Thus with asthma: in 2016, a literature review by the Cochrane collaboration judged that vitamin D seemed to reduce the risk of asthma attacks; but seven years later, in February 2023, the same authors updated their work and did not find proof of this protection.
Epidemiologists from the International Prevention Research Institute (Ipri), in Lyon, estimated, after a major literature review carried out around ten years ago, that, for all non-skeletal diseases, a low level of vitamin D was only a biological marker of deteriorated health, not its cause. In 2022, the HCSP delivered the same conclusion: “Drug supplementation trials have not yet made it possible to confirm a positive (or deleterious) effect on most pathologies potentially associated with vitamin D insufficiency in the general population. »
Among children, there is rather consensus on the need for supplementation, particularly among toddlers, who should not be exposed to the sun. French experts have published new recommendations in 2022, calling for daily supplementation until the age of 2, then ideally daily or, failing that, quarterly until the age of 18. But even this supplementation raises questions about its real effectiveness, indicates a meta-analysis by the Cochrane collaboration carried out in 2019.
In adults, vitamin D may be recommended in a few specific clinical situations (defects in mineralization or bone density, renal insufficiency, risk of falls in the elderly, pathologies or medications affecting metabolism, etc.). But “systematic drug supplementation with vitamin D in the general population is not possible given the current state of knowledge,” insists the HCSP. If you are an adult in good general health, with reasonable access to daylight, supplementation is unnecessary.
Cases of toxicity have been exceptionally reported. Thus, in 2019, Canadian nephrologists described the case of a 54-year-old man who suffered kidney failure after taking high doses of vitamin D (8,000 to 12,000 international units per day, or 2 to 3 times l tolerable maximum intake, according to health authorities and learned societies). Cases of overdose in children have also been reported with alerts from the Medicines Agency in 2021, then in 2023, linked to the taking of food supplements and which may have led to the hospitalization of previously healthy infants. After the Second World War, sporadic epidemics of vitamin D poisoning could also be observed in children whose milk was fortified.
Fortunately rare cases. “The risks of acute vitamin D poisoning, apart from exceptional pathologies, are practically zero,” notes the HCSP. On the other hand, there is a lack of data on possible negative effects of high doses administered regularly over the medium and long term. »

 B:SM will break its investment record this year with 62 million euros
B:SM will break its investment record this year with 62 million euros War in Ukraine: when kyiv attacks Russia with inflatable balloons loaded with explosives
War in Ukraine: when kyiv attacks Russia with inflatable balloons loaded with explosives United States: divided on the question of presidential immunity, the Supreme Court offers respite to Trump
United States: divided on the question of presidential immunity, the Supreme Court offers respite to Trump Maurizio Molinari: “the Scurati affair, a European injury”
Maurizio Molinari: “the Scurati affair, a European injury” Beware of the three main sources of poisoning in children
Beware of the three main sources of poisoning in children First three cases of “native” cholera confirmed in Mayotte
First three cases of “native” cholera confirmed in Mayotte Meningitis: compulsory vaccination for babies will be extended in 2025
Meningitis: compulsory vaccination for babies will be extended in 2025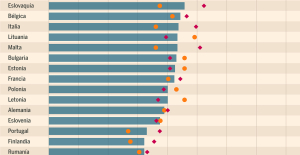 Spain is the country in the European Union with the most overqualified workers for their jobs
Spain is the country in the European Union with the most overqualified workers for their jobs In the United States, a Boeing 767 loses its emergency slide shortly after takeoff
In the United States, a Boeing 767 loses its emergency slide shortly after takeoff The A13 motorway will not reopen on May 1
The A13 motorway will not reopen on May 1 More than 1,500 items for less than 1 euro: the Dutch discounter Action opens a third store in Paris
More than 1,500 items for less than 1 euro: the Dutch discounter Action opens a third store in Paris 100 million euros in loans, water storage, Ecophyto plan… New measures from the executive towards farmers
100 million euros in loans, water storage, Ecophyto plan… New measures from the executive towards farmers New York justice returns 30 works of art looted from Cambodia and Indonesia
New York justice returns 30 works of art looted from Cambodia and Indonesia Les Galons de la BD dedicates War Photographers, a virtuoso album on the Spanish War
Les Galons de la BD dedicates War Photographers, a virtuoso album on the Spanish War Theater: Kevin, or the example of an academic failure
Theater: Kevin, or the example of an academic failure The eye of the INA: Jean Carmet, the thirst for life of a great actor
The eye of the INA: Jean Carmet, the thirst for life of a great actor Skoda Kodiaq 2024: a 'beast' plug-in hybrid SUV
Skoda Kodiaq 2024: a 'beast' plug-in hybrid SUV Tesla launches a new Model Y with 600 km of autonomy at a "more accessible price"
Tesla launches a new Model Y with 600 km of autonomy at a "more accessible price" The 10 best-selling cars in March 2024 in Spain: sales fall due to Easter
The 10 best-selling cars in March 2024 in Spain: sales fall due to Easter A private jet company buys more than 100 flying cars
A private jet company buys more than 100 flying cars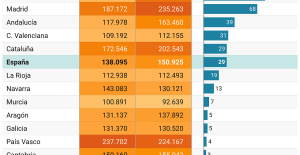 This is how housing prices have changed in Spain in the last decade
This is how housing prices have changed in Spain in the last decade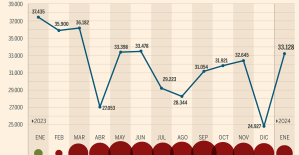 The home mortgage firm drops 10% in January and interest soars to 3.46%
The home mortgage firm drops 10% in January and interest soars to 3.46% The jewel of the Rocío de Nagüeles urbanization: a dream villa in Marbella
The jewel of the Rocío de Nagüeles urbanization: a dream villa in Marbella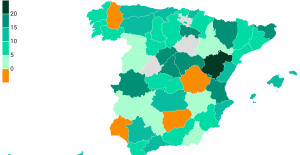 Rental prices grow by 7.3% in February: where does it go up and where does it go down?
Rental prices grow by 7.3% in February: where does it go up and where does it go down? Even on a mission for NATO, the Charles-de-Gaulle remains under French control, Lecornu responds to Mélenchon
Even on a mission for NATO, the Charles-de-Gaulle remains under French control, Lecornu responds to Mélenchon “Deadly Europe”, “economic decline”, immigration… What to remember from Emmanuel Macron’s speech at the Sorbonne
“Deadly Europe”, “economic decline”, immigration… What to remember from Emmanuel Macron’s speech at the Sorbonne Sale of Biogaran: The Republicans write to Emmanuel Macron
Sale of Biogaran: The Republicans write to Emmanuel Macron Europeans: “All those who claim that we don’t need Europe are liars”, criticizes Bayrou
Europeans: “All those who claim that we don’t need Europe are liars”, criticizes Bayrou These French cities that will boycott the World Cup in Qatar
These French cities that will boycott the World Cup in Qatar Toulouse-Racing 92: The liberating entry of Antoine Dupont, the Ile-de-France shipwreck... The tops and the flops
Toulouse-Racing 92: The liberating entry of Antoine Dupont, the Ile-de-France shipwreck... The tops and the flops Premier League: Sheffield United relegated after heavy defeat against Newcastle
Premier League: Sheffield United relegated after heavy defeat against Newcastle Judo: Audrey Tcheuméo consoles herself with a 5th European coronation
Judo: Audrey Tcheuméo consoles herself with a 5th European coronation Tennis: in Madrid, Rafael Nadal wins his revenge against Alex De Minaur
Tennis: in Madrid, Rafael Nadal wins his revenge against Alex De Minaur