is The nightmare for the more than 40000 people in Switzerland every year, to the reality of a cancer diagnosis. Thanks to modern methods of treatment of a cancer is a disease but not a death sentence anymore. However, the path to the right treatment can be rocky. Because of the normal run of the remuneration of anti-cancer drugs via the so-called specialties list is becoming more and more the exception.
Is a drug on this list, so the health insurance companies have to pay for it. But it is to be a means outside of the specialties listed indication is used or wants to use a doctor not in Switzerland, certified funds, he can apply for the compensation at the time of checkout as an exception case, which is called "as an compound of remuneration". Is regulated by this process in the article 71 of the regulation on the health insurance. The Fund may approve the use of Medicines. You can also say no.
extent unknown
"30 percent of all cancer are paid for treatments, in the meantime, as an compound, and the trend is rising," says Franziska Lenz, head of policy & Public Affairs, the Swiss cancer League. "As for children, almost 100 percent, because the medicine is only approved for adults and the remuneration of the specialty list based on it." How big is the Problem, weiss currently no one. The Federal office for health (BAG) was last collected in 2014 data on the number of as an compound of remuneration, currently a new survey is running. In 2014 there were between 6000 and 8000 cases. "In Switzerland, we estimate the number of all the indications, cross-currently around 25000 to 30000 cases," says Oliver Bleck, General Manager of Roche Pharma Switzerland.
Alone, Roche had been affected in the past year, with approximately 5500 cases of as an compound of remuneration. "In the case of the health insurers, the managers report a significant increase in cases in the last five years," confirms Andreas Schiesser, a collective bargaining expert at the health insurance Association of Curafutura.
For patients, the trend is tricky. "There are differences in how funds react to as an compound applications," says Prof. Markus Borner, Co-President of the Oncology society. "We often hear complaints that the coffers at the time of approving the Costs very in different ways," confirmed Franziska Lenz of the cancer League. "Whether a patient or a Patient with the same diagnosis gets treatment paid for or not, depends on his cash register, as well as by the Canton. This is unacceptable," says Lenz.
"Common guidelines"
The funds fight back: A difference in treatment there. "There are common policies and standardized assessment templates were developed by the society of trust doctors," says Marianne Eggenberger, project Manager for medicines when health insurance Association, Santésuisse. She admits, however: each time the application is "an individual assessment".
the oncologist Borner has already collected rejections. So he wanted to treat a couple of years ago a patient who suffered from pancreatic cancer, according to a pre-treatment with the cancer drug Abraxane. However, the agent is only approved as a first-line therapy, i.e. without pretreatment. The cashier of the patients refused to accept the compensation approved Alternatives available. "And that wasn't true, there was still no Alternative," says Borner. He, however, warns against General Fund bashing: The insurers are in the as an compound of remuneration in a difficult Situation. "Because of the trust doctor of the Fund must approve a drug application, for which there is no data on the efficacy," he explains. "And the criterion of cost-effectiveness is plentiful nebulous."
But why the number of as an compound of increases in compensation so strong? The population is ageing. In addition, new funds will be approved earlier and earlier, often on the Basis of Phase II data, explains Santésuisse expert, Eggenberger. And then the price takes a poker between the Federal office of public health and the industry for innovations, getting longer and longer. The hassle about the price for Roche's cancer drug Perjeta about went through the media.
rigid Grid
not more but most importantly keep the price formation process, with the treatment of reality seems to step. "The Trend in the treatment of cancer is that the Tumor can become more differentiated, and thus treated specifically diagnosed," says Franziska Lenz of the cancer League. "However, the indications from the specialties list are too narrow. The result is that new forms of treatment are not recorded, and then as an compound to be remunerated."
Roche Manager Bleck confirmed: "In 90 percent of cases, in which our medicines are used in article 71, have specialist doctors prescribed for you, on the approved indication." A prominent example is the cancer drug Mabthera, which was often used for rare blood cancer types for which the means was effective, but not officially approved.
adjustments required
Doctors and patients ' representatives are, in principle, happy to get thanks to article 71 still available Treatment options approved. But also Santésuisse sees the danger, "that, in addition to the specialties list is a lack of transparent and elaborate parallel system". Roche complained that the group learns nothing about whether the use of its resources outside of the official admission success. Here is important Knowledge is lost. "And it can't be that innovations are increasingly paid outside the specialty list, eligibility and remuneration processes need to develop further", writes Bleck.
"today's laws about how drugs and are paid approved, not more work," says Franziska Lenz. "We are currently evaluating the Problem and make any necessary Changes", it means from the Federal office of public health. Explosive: the office does not know what the funds for a as an compound of-compensation numbers.
(editing Tamedia)
Created: 13.05.2019, 22:50 PM

 After 13 years of mission and seven successive leaders, the UN at an impasse in Libya
After 13 years of mission and seven successive leaders, the UN at an impasse in Libya Germany: search of AfD headquarters in Lower Saxony, amid accusations of embezzlement
Germany: search of AfD headquarters in Lower Saxony, amid accusations of embezzlement Faced with Iran, Israel plays appeasement and continues its shadow war
Faced with Iran, Israel plays appeasement and continues its shadow war Iran-Israel conflict: what we know about the events of the night after the explosions in Isfahan
Iran-Israel conflict: what we know about the events of the night after the explosions in Isfahan China's GDP grows 5.3% in the first quarter, more than expected
China's GDP grows 5.3% in the first quarter, more than expected Alert on the return of whooping cough, a dangerous respiratory infection for babies
Alert on the return of whooping cough, a dangerous respiratory infection for babies Can relaxation, sophrology and meditation help with insomnia?
Can relaxation, sophrology and meditation help with insomnia? WHO concerned about spread of H5N1 avian flu to new species, including humans
WHO concerned about spread of H5N1 avian flu to new species, including humans Vacation departures and returns: with the first crossovers, heavy traffic is expected this weekend
Vacation departures and returns: with the first crossovers, heavy traffic is expected this weekend “Têtu”, “Ideat”, “The Good Life”… The magazines of the I/O Media group resold to several buyers
“Têtu”, “Ideat”, “The Good Life”… The magazines of the I/O Media group resold to several buyers The A13 motorway closed in both directions for an “indefinite period” between Paris and Normandy
The A13 motorway closed in both directions for an “indefinite period” between Paris and Normandy The commitment to reduce taxes of 2 billion euros for households “will be kept”, assures Gabriel Attal
The commitment to reduce taxes of 2 billion euros for households “will be kept”, assures Gabriel Attal The exclusive Vespa that pays tribute to 140 years of Piaggio
The exclusive Vespa that pays tribute to 140 years of Piaggio Kingdom of the great maxi scooters: few and Kymco wants the crown of the Yamaha TMax
Kingdom of the great maxi scooters: few and Kymco wants the crown of the Yamaha TMax A complaint filed against Kanye West, accused of hitting an individual who had just attacked his wife
A complaint filed against Kanye West, accused of hitting an individual who had just attacked his wife In Béarn, a call for donations to renovate the house of Henri IV's mother
In Béarn, a call for donations to renovate the house of Henri IV's mother Skoda Kodiaq 2024: a 'beast' plug-in hybrid SUV
Skoda Kodiaq 2024: a 'beast' plug-in hybrid SUV Tesla launches a new Model Y with 600 km of autonomy at a "more accessible price"
Tesla launches a new Model Y with 600 km of autonomy at a "more accessible price" The 10 best-selling cars in March 2024 in Spain: sales fall due to Easter
The 10 best-selling cars in March 2024 in Spain: sales fall due to Easter A private jet company buys more than 100 flying cars
A private jet company buys more than 100 flying cars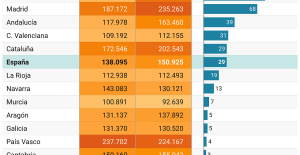 This is how housing prices have changed in Spain in the last decade
This is how housing prices have changed in Spain in the last decade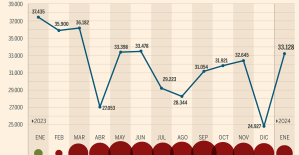 The home mortgage firm drops 10% in January and interest soars to 3.46%
The home mortgage firm drops 10% in January and interest soars to 3.46% The jewel of the Rocío de Nagüeles urbanization: a dream villa in Marbella
The jewel of the Rocío de Nagüeles urbanization: a dream villa in Marbella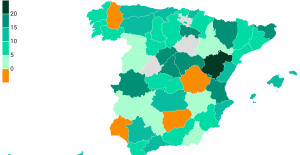 Rental prices grow by 7.3% in February: where does it go up and where does it go down?
Rental prices grow by 7.3% in February: where does it go up and where does it go down? With the promise of a “real burst of authority”, Gabriel Attal provokes the ire of the opposition
With the promise of a “real burst of authority”, Gabriel Attal provokes the ire of the opposition Europeans: the schedule of debates to follow between now and June 9
Europeans: the schedule of debates to follow between now and June 9 Europeans: “In France, there is a left and there is a right,” assures Bellamy
Europeans: “In France, there is a left and there is a right,” assures Bellamy During the night of the economy, the right points out the budgetary flaws of the macronie
During the night of the economy, the right points out the budgetary flaws of the macronie These French cities that will boycott the World Cup in Qatar
These French cities that will boycott the World Cup in Qatar Women's C1: at what time and on which channel to watch the OL-PSG semi-final first leg
Women's C1: at what time and on which channel to watch the OL-PSG semi-final first leg Tennis: after two victories this Friday, Grégoire Barrère qualifies for the semi-finals of the Bucharest tournament
Tennis: after two victories this Friday, Grégoire Barrère qualifies for the semi-finals of the Bucharest tournament Cycling: Mathieu Van der Poel “recharged the batteries” for Liège-Bastogne-Liège
Cycling: Mathieu Van der Poel “recharged the batteries” for Liège-Bastogne-Liège Mercato: Zidane at Bayern? We'll talk about it again, but...
Mercato: Zidane at Bayern? We'll talk about it again, but...


















