Covid-19 patients still have a slightly increased risk of some psychiatric and neurological problems two years after infection. This is what British researchers report in the journal “The Lancet Psychiatry” after evaluating the medical records of 1.28 million Covid 19 patients and a similar number of people with another respiratory disease.
The University of Oxford team led by Paul Harrison and Maxime Taquet used data from the US, UK, Spain, Bulgaria, Australia, India, Malaysia and Taiwan. During the comparison, the researchers made sure that the group of Covid patients and the control group with other respiratory diseases were very similar in terms of age, gender, ethnic origin and other characteristics. The Covid diseases were diagnosed between January 2020 and April 2022.
The results initially contradict the suspicion that Covid can cause long-term mood disorders. "It is good news that the excess of depression and anxiety diagnoses in the wake of Covid-19 is short-lived and not seen in children," Harrison said in a statement from his university.
Accordingly, mood disorders were at the same level as in the control group 43 days after the Covid diagnosis, and this was the case for anxiety disorders after 58 days. The scientists did not find an increased occurrence of such disorders in the age group under 18 years.
However, the study in Covid-19 patients indicates a slightly higher risk of clouded consciousness (brain fog), dementia, psychotic flare-ups and epilepsy even at the end of the two-year follow-up period. Calculated per 10,000 patients, there were 640 cases of impaired consciousness in the Covid group of 18 to 64 year olds, while there were 550 cases in the control group. In the over 64-year-olds, there were 450 cases of dementia in 10,000 Covid patients, in the control group there were 330 cases.
Researchers also looked at the effects of the alpha, delta and omicron coronavirus variants. Compared to the alpha variant, the delta variant showed an increased risk of ischemic stroke, epilepsy, impaired consciousness, insomnia and anxiety disorders. In the case of the omicron variant, there were therefore hardly any differences to the delta variant, but the death rate was lower.
"The results shed new light on the longer-term consequences for people's mental health and brain after a Covid-19 infection," says Taquet. However, the authors acknowledge that because of the database, Covid cases with little or no symptoms may be underrepresented.
It also did not take into account when the neurological or psychiatric diseases were first diagnosed and how severe the cases were. The team also admits that information about Covid diseases or vaccinations against the corona virus could be missing in the patient files, which could distort the results.
Jonathan Rogers and Glyn Lewis of University College London, who were not involved in the study, write in a comment, also in The Lancet Psychiatry: "This is the first study to attempt to explain some of the disparity in persistent neurological and psychiatric aspects of Covid-19 in a large data set.” Some clinical features require further examination.
The study is particularly relevant because of the enormous number of patients, the control group and the long observation period of two years, says Peter Berlit, Secretary General of the German Neurological Society (DGN). However, the validity is limited by the fact that the severity of the respiratory diseases in the control group was not taken into account.
The study does not show an increased risk of dementia in Covid patients. "It is known that latent dementia often becomes manifest as a result of a serious event, such as Covid-19 disease, without there being a causal connection," emphasizes the neurologist.

 Germany: Man armed with machete enters university library and threatens staff
Germany: Man armed with machete enters university library and threatens staff His body naturally produces alcohol, he is acquitted after a drunk driving conviction
His body naturally produces alcohol, he is acquitted after a drunk driving conviction Who is David Pecker, the first key witness in Donald Trump's trial?
Who is David Pecker, the first key witness in Donald Trump's trial? What does the law on the expulsion of migrants to Rwanda adopted by the British Parliament contain?
What does the law on the expulsion of migrants to Rwanda adopted by the British Parliament contain?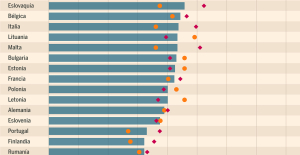 Spain is the country in the European Union with the most overqualified workers for their jobs
Spain is the country in the European Union with the most overqualified workers for their jobs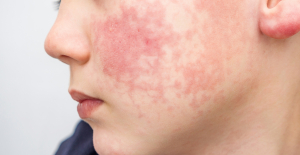 Parvovirus alert, the “fifth disease” of children which has already caused the death of five babies in 2024
Parvovirus alert, the “fifth disease” of children which has already caused the death of five babies in 2024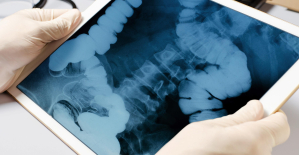 Colorectal cancer: what to watch out for in those under 50
Colorectal cancer: what to watch out for in those under 50 H5N1 virus: traces detected in pasteurized milk in the United States
H5N1 virus: traces detected in pasteurized milk in the United States Insurance: SFAM, subsidiary of Indexia, placed in compulsory liquidation
Insurance: SFAM, subsidiary of Indexia, placed in compulsory liquidation Under pressure from Brussels, TikTok deactivates the controversial mechanisms of its TikTok Lite application
Under pressure from Brussels, TikTok deactivates the controversial mechanisms of its TikTok Lite application “I can’t help but panic”: these passengers worried about incidents on Boeing
“I can’t help but panic”: these passengers worried about incidents on Boeing “I’m interested in knowing where the money that the State takes from me goes”: Bruno Le Maire’s strange pay slip sparks controversy
“I’m interested in knowing where the money that the State takes from me goes”: Bruno Le Maire’s strange pay slip sparks controversy 25 years later, the actors of Blair Witch Project are still demanding money to match the film's record profits
25 years later, the actors of Blair Witch Project are still demanding money to match the film's record profits At La Scala, Mathilde Charbonneaux is Madame M., Jacqueline Maillan
At La Scala, Mathilde Charbonneaux is Madame M., Jacqueline Maillan Deprived of Hollywood and Western music, Russia gives in to the charms of K-pop and manga
Deprived of Hollywood and Western music, Russia gives in to the charms of K-pop and manga Exhibition: Toni Grand, the incredible odyssey of a sculptural thinker
Exhibition: Toni Grand, the incredible odyssey of a sculptural thinker Skoda Kodiaq 2024: a 'beast' plug-in hybrid SUV
Skoda Kodiaq 2024: a 'beast' plug-in hybrid SUV Tesla launches a new Model Y with 600 km of autonomy at a "more accessible price"
Tesla launches a new Model Y with 600 km of autonomy at a "more accessible price" The 10 best-selling cars in March 2024 in Spain: sales fall due to Easter
The 10 best-selling cars in March 2024 in Spain: sales fall due to Easter A private jet company buys more than 100 flying cars
A private jet company buys more than 100 flying cars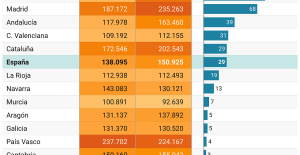 This is how housing prices have changed in Spain in the last decade
This is how housing prices have changed in Spain in the last decade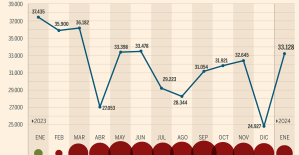 The home mortgage firm drops 10% in January and interest soars to 3.46%
The home mortgage firm drops 10% in January and interest soars to 3.46% The jewel of the Rocío de Nagüeles urbanization: a dream villa in Marbella
The jewel of the Rocío de Nagüeles urbanization: a dream villa in Marbella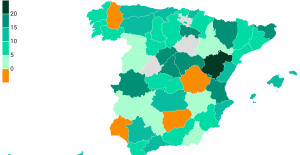 Rental prices grow by 7.3% in February: where does it go up and where does it go down?
Rental prices grow by 7.3% in February: where does it go up and where does it go down? Sale of Biogaran: The Republicans write to Emmanuel Macron
Sale of Biogaran: The Republicans write to Emmanuel Macron Europeans: “All those who claim that we don’t need Europe are liars”, criticizes Bayrou
Europeans: “All those who claim that we don’t need Europe are liars”, criticizes Bayrou With the promise of a “real burst of authority”, Gabriel Attal provokes the ire of the opposition
With the promise of a “real burst of authority”, Gabriel Attal provokes the ire of the opposition Europeans: the schedule of debates to follow between now and June 9
Europeans: the schedule of debates to follow between now and June 9 These French cities that will boycott the World Cup in Qatar
These French cities that will boycott the World Cup in Qatar Hand: Montpellier crushes Kiel and continues to dream of the Champions League
Hand: Montpellier crushes Kiel and continues to dream of the Champions League OM-Nice: a spectacular derby, Niçois timid despite their numerical superiority...The tops and the flops
OM-Nice: a spectacular derby, Niçois timid despite their numerical superiority...The tops and the flops Tennis: 1000 matches and 10 notable encounters by Richard Gasquet
Tennis: 1000 matches and 10 notable encounters by Richard Gasquet Tennis: first victory of the season on clay for Osaka in Madrid
Tennis: first victory of the season on clay for Osaka in Madrid


















